Unveiling The DO And MD Difference: Discoveries And Insights
Definition and example of "do and md difference"
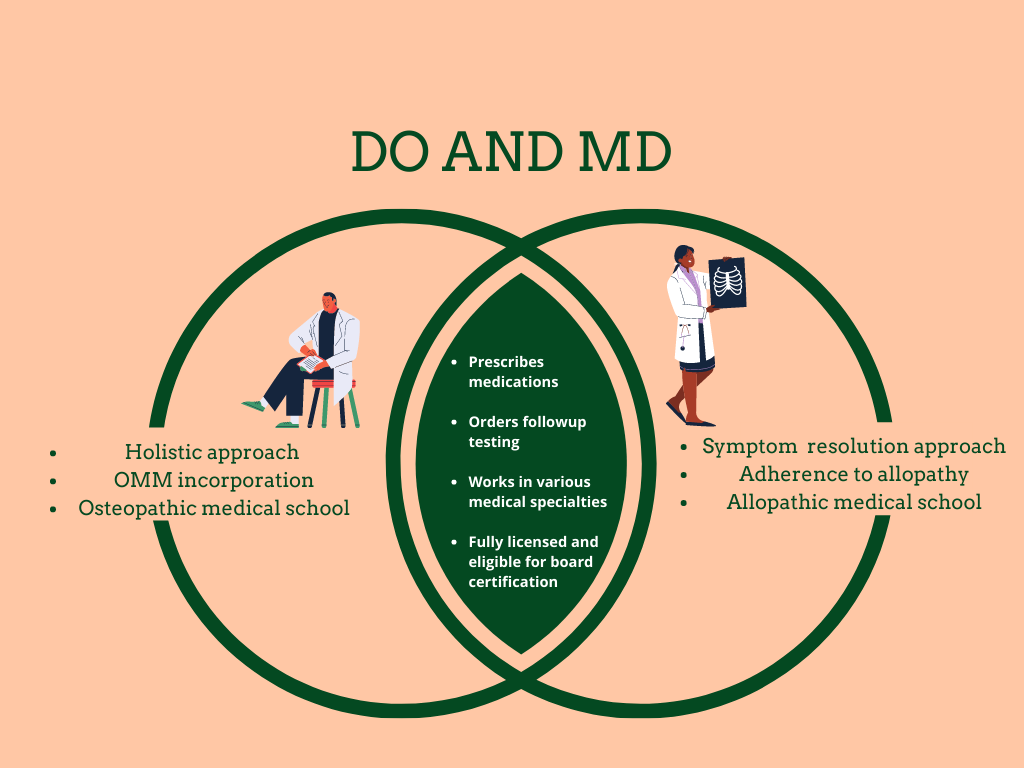
A distinction between a Doctor of Osteopathic Medicine (DO) and a Doctor of Medicine (MD) lies in their training and approach to patient care. DOs receive additional training in osteopathic manipulative treatment (OMT), a hands-on technique that focuses on the musculoskeletal system. While MDs primarily focus on pharmacological interventions, DOs emphasize holistic care, considering the physical, mental, and emotional well-being of their patients.
Importance, benefits, and historical context
The "DO and MD difference" is significant because it offers patients a choice in their healthcare providers. DOs' unique training allows them to provide comprehensive care, often reducing the need for additional specialists. Historically, DOs have played a vital role in rural and underserved communities, providing primary care to those who might otherwise lack access to healthcare.
Transition to main article topics
In the following sections, we will explore the "DO and MD difference" in more detail, examining their training, scope of practice, and respective contributions to the healthcare system. We will also discuss the factors patients may consider when choosing between a DO and an MD.
DO and MD Difference
The DO and MD difference encompasses various dimensions that shape the roles and approaches of these healthcare professionals. Here are 10 key aspects that explore these differences:
- Training: DOs receive additional training in osteopathic manipulative treatment (OMT).
- Scope of Practice: DOs have a broader scope of practice, including OMT and pharmacological interventions.
- Patient Care: DOs emphasize holistic care, considering the physical, mental, and emotional well-being of their patients.
- History: DOs have a long history of serving rural and underserved communities.
- Education: DOs and MDs attend different medical schools and receive distinct training.
- Licensing: DOs and MDs must pass separate licensing exams to practice medicine.
- Collaboration: DOs and MDs often collaborate to provide comprehensive patient care.
- Research: DOs and MDs conduct research to advance medical knowledge and improve patient outcomes.
- Recognition: DOs and MDs are both recognized as licensed physicians in the United States.
- Patient Choice: Patients have the choice to select a DO or MD based on their individual healthcare needs.
These key aspects highlight the unique contributions of DOs and MDs to the healthcare system. Their distinct training and approaches allow them to provide diverse and complementary care to patients. Understanding these differences empowers patients to make informed decisions about their healthcare providers.
Training
The additional training that DOs receive in osteopathic manipulative treatment (OMT) is a key component of the "DO and MD difference." OMT is a hands-on technique that focuses on the musculoskeletal system. DOs use OMT to diagnose and treat a variety of conditions, including back pain, neck pain, headaches, and sports injuries. OMT can also be used to improve overall health and well-being.
The inclusion of OMT in the training of DOs gives them a unique set of skills that can benefit patients. Studies have shown that OMT can be effective in reducing pain, improving range of motion, and decreasing the need for medication. OMT can also be used to prevent injuries and promote overall health.
The "DO and MD difference" is important for patients to understand because it can help them make informed decisions about their healthcare. Patients who are looking for a comprehensive approach to care may want to consider seeing a DO. DOs are trained to treat the whole person, not just the symptoms of an illness. They can use OMT to address the underlying causes of pain and dysfunction, and they can work with patients to develop personalized treatment plans that meet their individual needs.
Scope of Practice
The broader scope of practice for DOs, encompassing both osteopathic manipulative treatment (OMT) and pharmacological interventions, is a pivotal aspect of the "DO and MD difference." OMT, a hands-on technique, enables DOs to address musculoskeletal issues directly, complementing their ability to prescribe medications, order diagnostic tests, and perform procedures. This comprehensive approach empowers DOs to treat a wide range of conditions, including those that may not respond solely to medication or surgery.
The integration of OMT into a DO's practice offers several advantages. Firstly, it allows for a more holistic approach to patient care, considering the interplay between the musculoskeletal system and overall health. OMT can alleviate pain, improve mobility, and enhance the body's self-healing mechanisms. Secondly, OMT can reduce the need for opioids or other pain medications, promoting safer and more effective pain management. Thirdly, OMT can complement other therapies, such as physical therapy or chiropractic care, providing a synergistic approach to rehabilitation.
In practical terms, the broader scope of practice for DOs enables them to serve as primary care physicians, managing a diverse range of health concerns. They can provide comprehensive care, from preventive checkups to chronic disease management and acute injury treatment. DOs are also well-suited for roles in osteopathic manipulative medicine, sports medicine, and pain management clinics.
Patient Care
The emphasis on holistic care by DOs is a defining aspect of the "DO and MD difference." Holistic care considers the whole person, not just the symptoms of an illness. DOs are trained to understand the interconnectedness of the physical, mental, and emotional aspects of health. This approach allows them to treat the root causes of illness and promote overall well-being.
For example, a patient with chronic pain may be prescribed medication by an MD to manage the pain. A DO, on the other hand, may take a more holistic approach, considering the patient's lifestyle, stress levels, and emotional state. The DO may use OMT to address musculoskeletal imbalances that may be contributing to the pain. They may also recommend stress-reducing techniques or refer the patient to a therapist to address any emotional factors that may be exacerbating the pain.
The holistic approach of DOs can lead to better patient outcomes. Studies have shown that patients who receive holistic care are more likely to experience improved health and well-being. They are also more likely to be satisfied with their care and to adhere to their treatment plans.
The emphasis on holistic care is a key differentiator between DOs and MDs. Patients who are looking for a comprehensive and patient-centered approach to care may want to consider seeing a DO.
History
The historical connection between DOs and underserved communities significantly contributes to the "DO and MD difference." Osteopathic medicine originated in the late 19th century as a response to the lack of healthcare access in rural and underserved areas. DOs were trained to provide comprehensive care, including OMT, to communities that often lacked access to traditional medical services.
This historical legacy of service has shaped the values and priorities of DOs today. Many DOs choose to practice in rural and underserved areas, continuing the tradition of providing care to those who need it most. They play a vital role in addressing health disparities and improving access to healthcare in these communities.
Understanding this historical connection helps us appreciate the unique contributions of DOs to the healthcare system. Their commitment to serving underserved populations is a testament to their dedication to providing equitable and compassionate care.
Education
The distinct educational paths of DOs and MDs form a crucial component of the "DO and MD difference." DOs attend osteopathic medical schools, while MDs attend allopathic medical schools. This difference in education results in distinct training experiences that shape the professional identities and approaches of these healthcare providers.
Osteopathic medical schools emphasize a holistic and patient-centered approach to medicine. DOs receive comprehensive training in osteopathic manipulative treatment (OMT), a hands-on technique used to diagnose and treat musculoskeletal dysfunctions. This unique aspect of their education equips DOs with a broader skill set, enabling them to address the physical, mental, and emotional aspects of a patient's health.
The practical significance of this educational difference lies in the diversity of healthcare services that DOs can provide. Their training in OMT allows them to offer a range of non-invasive treatments, including pain management, injury rehabilitation, and preventive care. This comprehensive approach often complements traditional medical interventions, providing patients with a more integrative healthcare experience.
Understanding the educational distinction between DOs and MDs empowers patients to make informed decisions about their healthcare providers. Patients seeking a holistic and patient-centered approach to care may find that DOs align well with their preferences. The unique training and skills of DOs contribute significantly to the "DO and MD difference," shaping their roles as comprehensive healthcare providers.
Licensing
The separate licensing exams that DOs and MDs must pass to practice medicine underscore the "DO and MD difference." These exams ensure that both groups of healthcare professionals meet the necessary standards of knowledge and competence before providing patient care.
The licensing process for DOs and MDs involves rigorous training, comprehensive examinations, and ongoing continuing medical education. By successfully completing these requirements, DOs and MDs demonstrate their dedication to providing safe and effective patient care.
The practical significance of this licensing distinction lies in the assurance it provides to patients. When seeking medical care, patients can trust that both DOs and MDs have undergone rigorous training and met the required standards to practice medicine. This ensures a high level of professionalism and competence within the medical community.
Understanding the separate licensing requirements for DOs and MDs empowers patients to make informed decisions about their healthcare providers. By recognizing the distinct training and qualifications of each group, patients can choose the healthcare professional who best aligns with their individual needs and preferences.
Collaboration
This aspect of the "DO and MD difference" highlights the cooperative relationship between DOs and MDs in delivering comprehensive healthcare to patients. Collaboration between these two groups of healthcare professionals optimizes patient outcomes and ensures a holistic approach to patient care.
- Complementary Skills and Expertise: DOs' emphasis on OMT and holistic care complements MDs' focus on pharmacological interventions and disease management. This diversity of skills allows them to address a wide range of patient needs, providing a more comprehensive and integrated approach to healthcare.
- Shared Commitment to Patient Care: Despite their distinct training, DOs and MDs share a common goal of providing high-quality patient care. They work together to develop individualized treatment plans, combining their expertise to deliver the best possible outcomes for their patients.
- Improved Patient Outcomes: Collaborative care models involving DOs and MDs have been shown to improve patient outcomes. Studies indicate that patients who receive care from both DOs and MDs experience better pain management, reduced hospital stays, and enhanced overall health.
- Enhanced Patient Experience: Collaboration between DOs and MDs fosters a better patient experience. Patients benefit from access to a broader range of treatment options and the expertise of both types of healthcare professionals, leading to increased satisfaction and improved health outcomes.
In summary, the collaboration between DOs and MDs is a key aspect of the "DO and MD difference." Their complementary skills, shared commitment to patient care, and positive impact on patient outcomes demonstrate the value of their collaborative approach in providing comprehensive and high-quality healthcare.
Research
The research contributions of DOs and MDs are integral to the "DO and MD difference," as both groups actively engage in scientific inquiry to enhance healthcare practices and improve patient outcomes. Their dedication to research underscores their commitment to staying abreast of the latest medical advancements and translating research findings into tangible benefits for patients.
- Collaborative Research: DOs and MDs often collaborate on research projects, combining their diverse perspectives and expertise to address complex medical challenges. This synergistic approach fosters innovation and leads to more comprehensive research outcomes.
- Translational Research: DOs and MDs are dedicated to translational research, which involves applying research findings directly to patient care. This ensures that new knowledge and technologies are swiftly incorporated into clinical practice, benefiting patients in a timely manner.
- Patient-Centered Research: DOs and MDs prioritize patient-centered research, actively involving patients in the research process. This participatory approach ensures that research is aligned with the needs and priorities of patients, leading to more relevant and impactful outcomes.
- Interdisciplinary Research: DOs and MDs recognize the value of interdisciplinary research, collaborating with researchers from other fields such as public health, engineering, and psychology. This cross-disciplinary approach allows for a more holistic understanding of health and disease, leading to novel solutions and improved patient care.
In summary, the research endeavors of DOs and MDs are a cornerstone of the "DO and MD difference." Their commitment to scientific inquiry, translational research, patient-centered approaches, and interdisciplinary collaboration drives medical progress and ultimately enhances patient outcomes.
Recognition
The recognition of DOs and MDs as licensed physicians in the United States is a critical component of the "DO and MD difference" and holds significant implications for healthcare delivery and patient care.
This recognition ensures that both DOs and MDs undergo rigorous training, pass comprehensive licensing exams, and adhere to the same standards of medical practice. It signifies that they are equally qualified to diagnose and treat medical conditions, prescribe medications, and perform medical procedures.
The practical significance of this recognition lies in the seamless integration of DOs and MDs into the healthcare system. They can practice in all medical settings, including hospitals, clinics, and private practices. Patients can confidently seek care from either DOs or MDs, knowing that they will receive high-quality, evidence-based medical care.
Furthermore, the recognition of DOs and MDs as licensed physicians promotes collaboration and interdisciplinary teamwork within the medical field. They can consult with each other, refer patients, and work together to provide comprehensive care. This collaborative approach benefits patients by ensuring they have access to the expertise of both types of healthcare professionals.
In summary, the recognition of DOs and MDs as licensed physicians in the United States is a crucial aspect of the "DO and MD difference." It ensures that both groups of healthcare professionals meet the same high standards of medical practice, can seamlessly integrate into the healthcare system, and can work collaboratively to provide optimal patient care.
Patient Choice
In the context of the "DO and MD difference," patient choice is paramount. Patients have the opportunity to select a healthcare provider who aligns with their unique healthcare needs and preferences. Understanding the differences between DOs and MDs empowers patients to make informed decisions about their care.
- Treatment Approach: Patients can choose a DO if they prefer a holistic approach to healthcare that emphasizes OMT and preventive care. Alternatively, they may select an MD if they prefer a more traditional approach focused on pharmacological interventions.
- Provider-Patient Relationship: Patients have the choice to select a healthcare provider with whom they feel comfortable and who understands their individual needs. DOs often prioritize building strong patient-physician relationships, while MDs may have a more clinical approach.
- Area of Expertise: Patients can consider the area of expertise when selecting a DO or MD. DOs often specialize in osteopathic manipulative medicine, sports medicine, and pain management, while MDs may specialize in a wider range of medical fields.
- Location and Availability: Patients may choose a DO or MD based on their location and availability. DOs are more likely to practice in rural and underserved areas, while MDs are more commonly found in urban areas.
By understanding the "DO and MD difference," patients can exercise their choice and select the healthcare provider who best meets their individual needs. This choice empowers patients and contributes to improved patient outcomes and satisfaction.
FAQs on "DO and MD Difference"
This section addresses commonly asked questions regarding the differences between Doctors of Osteopathic Medicine (DOs) and Doctors of Medicine (MDs), providing clear and informative answers to aid in understanding their distinct roles and approaches to patient care.
Question 1: What is the primary difference between a DO and an MD?
Answer: The primary difference lies in their training. DOs receive additional training in osteopathic manipulative treatment (OMT), a hands-on technique that focuses on the musculoskeletal system. This holistic approach allows DOs to address the physical, mental, and emotional well-being of their patients.
Question 2: Can DOs prescribe medications and perform surgeries?
Answer: Yes, DOs have the same scope of practice as MDs, including the ability to prescribe medications, perform surgeries, and order diagnostic tests. They are licensed to practice medicine and meet the same rigorous standards as MDs.
Question 3: Are DOs and MDs equally qualified to provide healthcare?
Answer: Yes, both DOs and MDs undergo comprehensive medical training and must pass licensing exams to practice medicine. They are both highly qualified to diagnose and treat medical conditions, providing safe and effective patient care.
Question 4: When should I choose a DO over an MD?
Answer: If you prefer a holistic approach to healthcare that emphasizes preventive care and hands-on treatment, a DO may be a suitable choice. DOs are particularly skilled in musculoskeletal medicine and often focus on promoting overall well-being.
Question 5: Can DOs and MDs work together to provide patient care?
Answer: Yes, DOs and MDs frequently collaborate to provide comprehensive patient care. They recognize the value of their complementary skills and often refer patients to each other for specialized treatment.
Question 6: Are DOs more likely to practice in rural areas?
Answer: Historically, DOs have had a strong presence in rural and underserved communities. While this trend is changing, DOs continue to play a vital role in providing healthcare access to those in need.
Summary: Understanding the "DO and MD difference" empowers patients to make informed decisions about their healthcare providers. Both DOs and MDs are qualified to provide high-quality medical care, with DOs offering a more holistic approach that emphasizes preventive care and osteopathic manipulative treatment.
Transition: This concludes our exploration of the "DO and MD difference." For further information or to find a DO or MD near you, please refer to the resources provided in the next section.
Understanding the "DO and MD Difference"
To effectively navigate the healthcare system and make informed decisions about your medical care, it is essential to understand the "DO and MD difference." Here are some key tips to guide you:
Tip 1: Recognize the Scope of PracticeDOs and MDs have similar scopes of practice, including the ability to diagnose and treat medical conditions, prescribe medications, and perform surgeries. However, DOs receive additional training in osteopathic manipulative treatment (OMT), a hands-on technique that focuses on the musculoskeletal system.Tip 2: Consider Your Healthcare NeedsWhen choosing between a DO and an MD, consider your individual healthcare needs and preferences. If you value a holistic approach to care that emphasizes preventive medicine and hands-on treatment, a DO may be a suitable choice. DOs are particularly skilled in musculoskeletal medicine and often focus on promoting overall well-being.Tip 3: Explore Their Training and QualificationsBoth DOs and MDs undergo rigorous medical training and must pass licensing exams to practice medicine. They are equally qualified to provide safe and effective patient care. Research their educational background, certifications, and areas of expertise to find a healthcare provider who aligns with your needs.Tip 4: Seek a Collaborative ApproachDOs and MDs often collaborate to provide comprehensive patient care. They recognize the value of their complementary skills and may refer patients to each other for specialized treatment. Encourage open communication and collaboration between your healthcare providers to ensure you receive the best possible care.Tip 5: Consider Their Availability and LocationThe availability and location of DOs and MDs can vary depending on the region and specialty. If you live in a rural or underserved area, you may have more limited access to DOs. Research the availability of healthcare providers in your area and consider their proximity to your residence or workplace.Summary: Understanding the "DO and MD difference" empowers you to make informed decisions about your healthcare. By considering your individual needs, researching their training and qualifications, seeking a collaborative approach, and considering their availability and location, you can find the right healthcare provider for you.Transition: For further information or to find a DO or MD near you, please refer to the resources provided in the next section.Conclusion
Throughout this article, we have explored the "DO and MD difference," examining the distinct training, approaches to care, and roles of Doctors of Osteopathic Medicine (DOs) and Doctors of Medicine (MDs) in the healthcare system. Understanding this difference empowers patients to make informed decisions about their healthcare providers and navigate the healthcare landscape effectively.
The holistic approach of DOs, with their emphasis on osteopathic manipulative treatment and preventive care, offers a unique perspective in patient care. DOs are particularly skilled in addressing musculoskeletal issues and promoting overall well-being. MDs, on the other hand, provide comprehensive medical care, specializing in a wide range of medical fields, often utilizing pharmacological interventions and surgical procedures.
It is important to note that both DOs and MDs are licensed physicians who undergo rigorous training and must meet the same high standards of medical practice. They work collaboratively to provide optimal patient care, recognizing the value of their complementary skills. Patients should consider their individual healthcare needs, preferences, and the availability of DOs and MDs in their area when making decisions about their healthcare providers.
The "DO and MD difference" highlights the diversity and expertise within the medical profession. By understanding these differences, patients can actively participate in their healthcare journey and choose the healthcare provider who best aligns with their unique needs. This informed decision-making ultimately leads to improved patient outcomes and a more personalized healthcare experience.